Losing a tooth doesn’t just change your smile — it starts a chain reaction that can weaken the jawbone and alter how your face looks and functions. You’ll learn how bone loss happens, why it matters for chewing and nearby teeth, and what options actually protect the jaw.
For those considering dental implants in Las Vegas, implants replace the tooth root and stimulate the bone, helping prevent the bone loss that follows missing teeth. You’ll also see who qualifies for implants, what the procedure involves, and when additional treatments might be needed to restore bone before or during implant placement.
Understanding Bone Loss and Its Impact on Oral Health
Bone loss in the jaw changes how your teeth, gums, and facial structure function. It affects chewing strength, tooth stability, and the fit of dentures, and increases risk for further tooth loss and infection.
Causes of Jawbone Deterioration
When you lose a tooth, the jawbone at that site stops receiving the mechanical stimulation it needs from chewing. Without that stimulus, your body resorbs bone tissue to conserve resources, and bone height and width shrink over months to years.
Periodontal (gum) disease causes chronic inflammation that destroys the bone supporting your teeth. Long-term infection, unmanaged tooth decay, and repeating extractions in the same area also accelerate bone loss. Systemic factors like uncontrolled diabetes, smoking, certain medications (for example, long-term corticosteroids), and osteoporosis can weaken bone quality and speed deterioration.
Consequences of Untreated Bone Loss
Bone loss reduces the vertical height and horizontal thickness of your jaw, which directly affects chewing efficiency and nutritional intake. Missing bone can make adjacent teeth mobile or lead to additional tooth loss because the supporting structure diminishes.
Facial appearance changes occur as the lower third of your face loses support: lips may collapse and cheeks appear sunken, which alters speech and facial proportions. Denture wearers often experience poor fit and sore spots because dentures rely on underlying bone and soft tissue that may be resorbed. Finally, severe bone loss can limit your options for tooth replacement and may require complex grafting procedures before implants are possible.
Signs and Symptoms of Bone Loss
Early bone loss can be painless, so you must watch for subtle signs. Look for increased tooth mobility, shifting or gaps between teeth, and changes in your bite or the way dentures sit.
You may notice receding gums, longer-looking teeth, or persistent bad breath and bleeding gums—common signs of periodontal disease. Radiographic findings on dental X-rays or CBCT scans reveal the most definitive evidence, showing reduced bone height and density around tooth roots or implant sites.
How Dental Implants Prevent Jawbone Loss
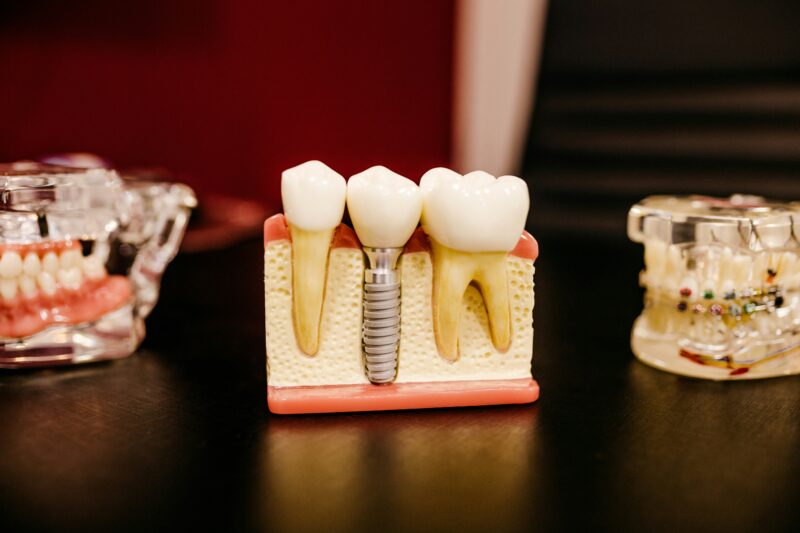
Dental implants replace missing tooth roots and restore the mechanical forces your jawbone needs to stay dense and shaped. They attach directly to bone, transmit bite forces, and support surrounding teeth and soft tissue to reduce the bone resorption that follows tooth loss.
Mechanism of Bone Stimulation
An implant is a titanium or ceramic screw placed into your jawbone. Bone cells respond to the micro-movements and load from chewing transmitted through the implant by maintaining or building bone — a process called mechanotransduction.
After placement, the bone grows tightly against the implant surface (osseointegration), creating a stable load-bearing interface. That stability lets you apply normal chewing forces to the implant-supported crown or bridge, which keeps osteoblast activity up and prevents the disuse resorption that occurs when a tooth root is missing.
You should expect some remodeling after surgery, but long-term functional loading preserves ridge height and width better than leaving the space empty. Proper placement, implant diameter and length, and timely restoration all influence how effectively stimulation preserves your bone.
Comparison With Other Tooth Replacement Options
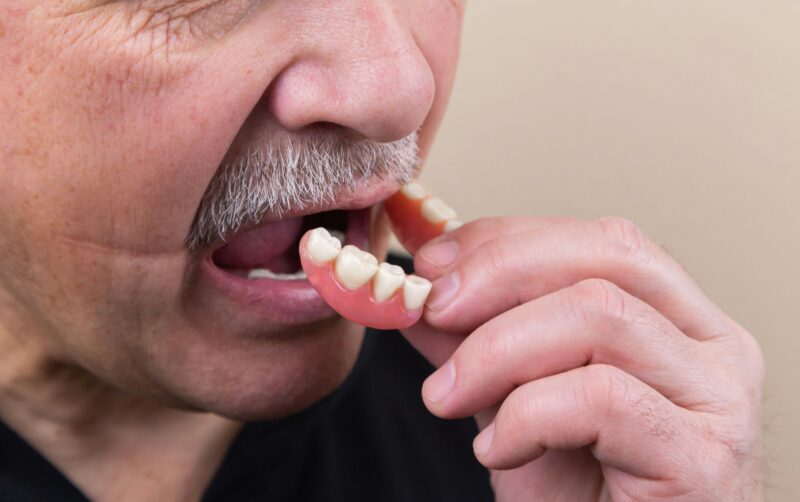
Removable dentures sit on the gum and do not transmit bite forces to the underlying bone. Over time your jaw beneath the denture will resorb, causing poor fit and progressive facial collapse.
Fixed bridges transfer some force to adjacent natural teeth rather than directly to bone. That preserves appearance and function but does not prevent localized bone loss at the missing-root site because the bone lacks direct stimulation.
Implants uniquely mimic a natural root by delivering load into the bone. If you want to prevent bone loss at the missing tooth site, implants provide the most direct and predictable mechanical stimulus compared with dentures or conventional bridges.
Long-Term Benefits for Jaw Structure
By preserving bone height and width, implants help maintain the original contours of your jaw and the position of neighboring teeth. That reduces future restorative needs such as bone grafting, angled implant placements, or altered prosthetic designs.
Maintained bone also supports your facial tissues, which lessens the progressive sagging and sunken appearance that can follow multiple missing teeth. Clinically, patients with well-integrated, regularly loaded implants show less vertical ridge loss over years than those wearing dentures.
To maximize long-term benefits, keep excellent oral hygiene, attend periodic implant check-ups, and avoid habits that overload or damage the implant, such as heavy smoking or bruxism without a nightguard.
Eligibility and Considerations for Dental Implant Placement
You will need adequate jaw bone, good gum health, and a review of medical history and medications to determine suitability. Smoking, uncontrolled systemic disease, and certain drugs can affect healing and implant success.
Assessing Bone Density and Volume
Your dentist or oral surgeon will measure bone height, width, and quality using CBCT scans and intraoral exams. These images show if the jaw has enough vertical height and horizontal thickness to hold a titanium implant without risking nerve or sinus injury.
If bone is thin or low-density, your provider evaluates implant diameter and length options and may recommend alternative sites or staged treatment. Expect measurement thresholds: many clinicians prefer at least 6–8 mm of bone width and 10 mm of height for standard implants, though narrower or shorter implants can be used in select cases.
Your bite forces, adjacent tooth support, and esthetic needs also guide planning. You should disclose prior extractions, trauma, or infections because those events influence localized bone loss patterns.
Bone Grafting and Regenerative Techniques
When bone is insufficient, grafting rebuilds volume using autograft, allograft, xenograft, or synthetic materials. Your surgeon matches graft type to the defect: block grafts for ridge width, particulate grafts for socket preservation, and sinus lifts for upper posterior height loss.
Guided bone regeneration (GBR) pairs grafts with resorbable or nonresorbable membranes to exclude soft tissue and promote bone growth. Healing times range from 3 to 9 months before implant placement, depending on graft material and site.
You should expect risks like infection, graft failure, or additional surgery, and smoking or uncontrolled diabetes raises those risks. Your clinician will review timelines, costs, and realistic expectations for functional and esthetic outcomes.