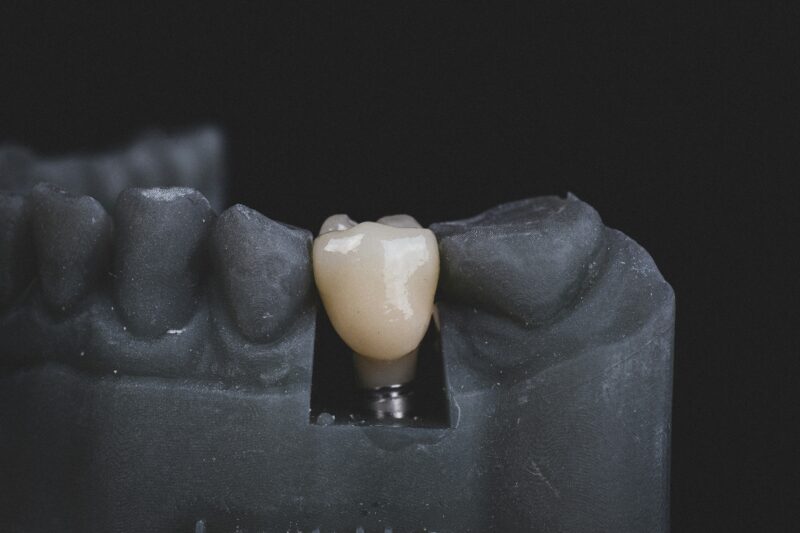
Missing teeth affect more than your smile—they change how you eat, speak, and feel about your appearance. Single tooth dental implants replace missing tooth roots with a stable, bone-integrated post and a natural-looking crown, giving you function and aesthetics closest to a real tooth.
If you want a durable option that preserves jawbone and avoids altering adjacent teeth, implants often fit the bill, though they require good oral health and a multi-step treatment plan. The sections ahead will explain how implants work, the benefits and risks, who makes a good candidate, and what to expect during the implant process so you can decide if this solution matches your goals.
Understanding Dental Implants
Dental implants replace missing tooth roots, support restorations like crowns or dentures, and can preserve jawbone structure and chewing function. You’ll learn what implants are, how they integrate with bone, and the main implant types you might encounter.
What Are Dental Implants?
A dental implant is a small, typically titanium, post surgically placed into your jawbone to serve as an artificial tooth root. An abutment connects the post to a visible restoration—most often a crown, bridge, or denture.
Manufacturers also produce implants in zirconia (ceramic) for metal-allergic or aesthetic needs. Implant systems vary by design (shape, thread) and surface treatment to improve bone integration.
Your clinician chooses implant size and material based on jawbone volume, location (front vs. back teeth), bite forces, and aesthetics. Proper planning, including X-rays or CBCT scans, helps match the implant to your anatomy and treatment goals.
How Dental Implants Work
After placement, the implant goes through osseointegration: bone grows tightly against the implant surface, stabilizing it as a functional root. This process typically takes 3–6 months, depending on bone quality and location.
Once integrated, the abutment and a custom restoration attach to the implant, restoring chewing, speech, and appearance.
You must maintain implants like natural teeth—daily brushing, flossing, and regular dental check-ups—to prevent peri-implantitis (inflammation and bone loss). Smoking, uncontrolled diabetes, and poor oral hygiene increase implant failure risk.
Types of Dental Implants
- Endosteal (in-bone): The most common type, placed directly into the jawbone. Suitable for single-tooth crowns, bridges, or implant-supported dentures.
- Subperiosteal (on-bone): A metal framework sits on the jawbone under the gum for patients with insufficient bone who cannot or prefer not to undergo bone grafting.
- Zygomatic implants: Longer implants anchored in the cheekbone for severely atrophic upper jaws where standard implants are not possible.
You’ll also encounter classifications by restoration type:
- Single implants for one missing tooth.
- Implant-supported bridges for adjacent missing teeth.
- Implant-retained or implant-supported dentures for full-arch replacement.
Discuss bone grafting, sinus lifts, or immediate (same-day) loading options with your dentist to determine which implant type fits your oral condition and timeline.
Benefits of Dental Implants
Dental implants restore chewing, speech, and the look of your smile while also protecting surrounding bone and teeth. They replace a tooth root with a stable anchor, support a realistic crown or denture, and often reduce the need for repeated dental work.
Improved Function and Appearance
Implants anchor a crown, bridge, or denture directly in your jawbone, so you regain chewing strength comparable to natural teeth. You can eat tougher foods—like apples and nuts—with less worry about slipping or pressure points that you might get from removable dentures.
The crown attached to an implant is matched to your tooth color and shape for a natural look. Because the implant supports the restoration from below, your lip and facial contours stay fuller than they often do with long-term tooth loss.
Long-Term Oral Health Advantages
An implant replaces the missing tooth root, which helps preserve the jawbone by transmitting chewing forces into bone and preventing resorption. This maintains the bone height and supports neighboring teeth, reducing the risk of shifting or bite changes.
You avoid altering adjacent healthy teeth, unlike some bridge procedures that require grinding down neighboring teeth for anchors. With proper brushing, flossing, and regular dental visits, implants lower the chance you’ll need additional restorative work on nearby teeth.
Durability and Reliability
Titanium or titanium-alloy implants integrate with bone (osseointegration), creating a stable base that can last decades with good care. Many implants remain functional for 15–30 years or longer when you maintain oral hygiene and attend periodic checkups.
Implant-supported restorations have predictable failure modes and repair options: if a crown wears or chips, the crown can be replaced without removing the implant. Smoking, uncontrolled diabetes, and poor oral hygiene increase risk, so you and your dentist should evaluate those factors before proceeding.
Candidacy and Suitability
Dental implants work best when you have stable oral health, adequate jawbone, and manageable medical conditions. The right candidate typically maintains good oral hygiene, can tolerate minor surgery, and has realistic expectations about timeline and costs.
Who Is a Good Candidate?
You qualify if you have one or more missing teeth and healthy gums free of untreated periodontal disease. Sufficient jawbone height and density at the implant site matter because implants rely on bone to fuse (osseointegration). Your dentist will evaluate bone using X-rays or a CBCT scan.
You should be able to undergo a minor surgical procedure and follow post-op care, including antibiotics and oral rinses when prescribed. Non-smokers or those willing to quit improve healing and long-term success. If you wear removable dentures, implants can often provide a fixed or more stable solution.
Factors Influencing Eligibility
Bone volume, gum health, and the location of missing teeth directly affect implant planning. Posterior (back) teeth sites often need more bone grafting than front teeth. The number and spacing of remaining teeth determine whether a single implant, bridge, or implant-supported denture fits best.
Lifestyle factors such as smoking, heavy alcohol use, and poor oral hygiene raise the risk of implant failure. Age alone rarely disqualifies you; many older adults receive implants successfully if bone and health permit. Financial considerations and willingness to complete a multi-month treatment plan also influence whether implants are a practical choice.
Medical Considerations
Systemic conditions can affect healing and infection risk. Uncontrolled diabetes, recent radiation to the head/neck, or autoimmune diseases may require medical clearance and careful coordination with your physician. Certain medications — especially bisphosphonates or immunosuppressants — change the risk profile and may necessitate alternative approaches.
Anticoagulant therapy and heart valve issues require preoperative planning with your dentist and prescribing physician. If you have osteoporosis or are on long-term steroids, your dentist may recommend additional imaging and modified surgical protocols. Always disclose full medical history, current medications, and supplements so your care team can tailor treatment to your specific health needs.
What to Expect From the Dental Implant Process
You will go through three main stages: careful planning with scans and a treatment plan; one or more surgical visits to place implants and possibly bone grafts; and a recovery period with temporary and final restorations. Each stage has predictable steps, typical timelines, and specific actions you’ll need to take.
Consultation and Planning
Your first visit focuses on assessment and imaging. Your dentist or oral surgeon will review medical history, medications, and any conditions that affect healing, such as diabetes or smoking. Expect digital X‑rays and a CBCT (3D) scan to measure bone volume and locate nerves and sinuses.
Your provider will discuss options—single implant, multiple implants, or implant‑retained dentures—and whether you need extra procedures like tooth extraction or bone grafting. They will present a treatment timeline, costs, and anesthesia choices (local, sedation, or general). Ask about success rates, warranties on components, and who will perform each step.
Surgical Procedure Overview
On surgery day you will receive anesthesia based on the plan. The surgeon makes a small incision in the gum, drills into the jawbone, and inserts a titanium implant post. If bone grafting or sinus lift is required, the graft may be placed at the same time or in a separate procedure.
After implant placement, your clinician often places a healing cap or temporary crown. If primary stability is strong, you might get a provisional restoration; if not, the site closes to heal beneath the gum. Typical healing (osseointegration) takes 3–6 months for the bone to fuse to the implant.
Recovery and Aftercare
Expect swelling, mild bleeding, and discomfort for 48–72 hours; your clinician will prescribe pain control and antibiotics if needed. Use ice packs, soft foods, and avoid smoking to support healing. Keep oral hygiene gentle around the surgical site—soft rinses and careful brushing.
Follow‑up visits check healing and remove sutures in 7–14 days. Once bone integration is confirmed, your clinician will expose the implant (if covered) and take impressions for the final abutment and crown. Maintain regular dental cleanings and avoid hard bites on the new restoration while it settles. Long‑term success depends on daily oral care and annual exams.