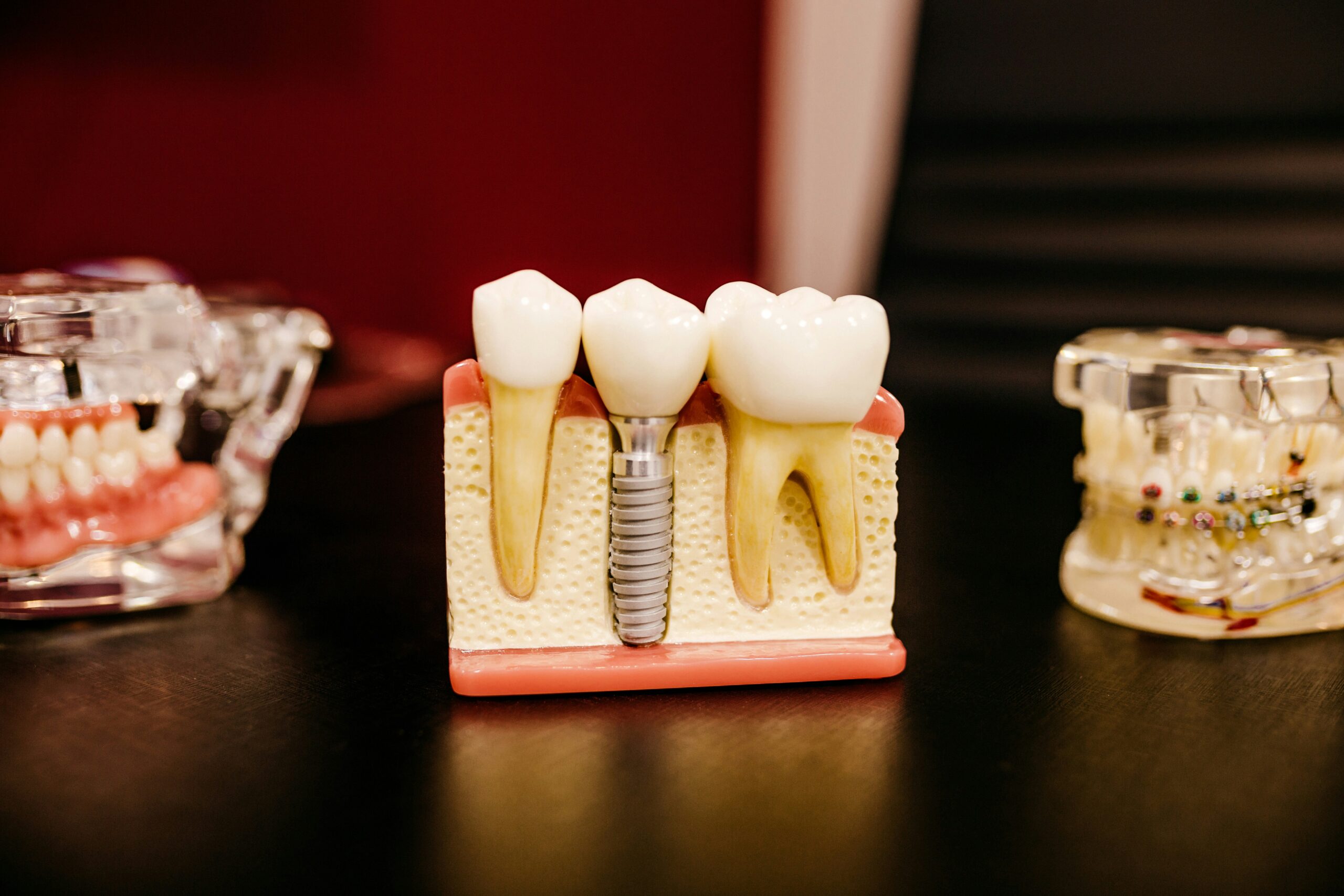
You may qualify for dental implants even if you worry about age, past dental work, or medical conditions. Your dentist checks specific health and anatomic factors to decide whether implants will be safe, predictable, and long-lasting for you. If you have good overall health, sufficient jawbone, and a commitment to oral hygiene, you are often a strong candidate for dental implants.
This post walks through the eligibility basics, the seven critical checks your dentist uses, advanced considerations that can affect candidacy, and options if you need preparatory care. Expect clear, practical information that helps you understand what your dentist will evaluate and what steps you can take next to pursue implants with confidence, especially when exploring dental implants in Cleveland Ohio as a long-term tooth replacement option.
Eligibility Basics for Dental Implants
You need enough bone support, stable overall health, and habits that won’t undermine healing. Your dentist evaluates jaw development, medical conditions, and lifestyle factors to decide if implants will integrate and last.
Age and Jawbone Development
Implants require fully developed jawbones. If you’re under 18–21 (varies by individual and jaw region), your dentist will likely delay implants until growth finishes to avoid implant position changes as the jaw continues to change.
If you’ve lost teeth long ago, bone volume often decreases. Your dentist will assess bone height and width with X-rays or a CBCT scan. If bone is insufficient, they may recommend bone grafting, sinus lift, or ridge augmentation before placing implants.
Older age alone is not a barrier. Many patients in their 60s, 70s, and beyond receive implants successfully when bone quality is adequate and medical risks are managed.
General Health Requirements
Your immune response and healing ability strongly affect implant success. Conditions like uncontrolled diabetes, certain autoimmune diseases, or recent cancer treatments raise infection and non‑integration risk. Your dentist will ask about medications, radiation history, and chronic illnesses.
You must be able to undergo minor oral surgery. That means reasonably controlled chronic conditions, acceptable blood clotting status, and no contraindicated cardiac or bleeding disorders. Your provider may coordinate with your physician to optimize health before surgery.
Medications such as bisphosphonates or immunosuppressants require special planning. Smokers and patients on high‑dose steroid therapy need extra precautions, monitoring, or alternative plans.
Lifestyle Habits That Affect Suitability
Tobacco use directly reduces implant success by impairing blood flow and healing. If you smoke or vape, your dentist will advise quitting several weeks before surgery and during healing; long‑term cessation significantly improves outcomes.
Poor oral hygiene and untreated gum disease increase failure risk. You must commit to daily brushing, flossing, and regular professional cleanings; your dentist will treat periodontal disease before implant placement.
Bruxism (teeth grinding) and heavy alcohol use also threaten implant integrity. Your dentist may recommend a nightguard, behavior modification, or staged treatment to protect implants and ensure predictable long‑term function.
What Your Dentist Checks: 7 Critical Factors
Your dentist evaluates bone support, gum health, medical issues, and medications because these directly affect implant stability, healing, and long-term success. Expect specific tests and questions that guide whether implants need preparation steps like bone grafting or disease control.
Jawbone Density and Quality
Your dentist measures the height, width, and density of the jawbone where the implant will go. They use CBCT scans or panoramic X-rays to see bone volume, the proximity of nerves and sinuses, and the direction of the ridge. Those images determine if the bone can hold an implant immediately or if grafting, sinus lift, or ridge augmentation is required.
If you’ve had a tooth removed long ago, the ridge may have resorbed; small defects can often be corrected, but severe loss changes the treatment plan. The dentist also considers bone quality (cortical vs. cancellous bone) because denser bone offers better initial stability.
Gum Health and Oral Hygiene
Your dentist checks for active gum disease, pocket depths, bleeding on probing, and the presence of plaque or calculus. Untreated periodontitis increases infection risk around an implant, so you must have controlled periodontal pockets and healthy soft tissue before surgery.
They assess how well you brush and floss and may recommend professional cleaning or a periodontal treatment plan first. If gum tissue is thin or recessed, soft-tissue grafts or papilla management strategies may be needed to achieve a stable, esthetic result.
Overall Health and Medical Conditions
Your dentist reviews chronic conditions such as diabetes, autoimmune disorders, osteoporosis, and heart disease because they affect healing and infection risk. Well-controlled type 2 diabetes usually allows implants, but high HbA1c values warrant stabilization before surgery.
Smoking, heavy alcohol use, and radiation to the head/neck also change candidacy; quitting smoking and coordinating care with your physician or oncologist improve outcomes. Your dentist may require medical clearances or collaborate with specialists for patients on immunosuppressants or with complex cardiac histories.
Medications and Their Impact
Tell your dentist about current and recent medications, especially bisphosphonates, anticoagulants, steroids, and immunosuppressants. Bisphosphonates and antiresorptives increase rare risks of osteonecrosis of the jaw; the dentist evaluates dose, duration, and route (oral vs. IV) before planning surgery.
Anticoagulants may require perioperative management with your prescriber to balance bleeding risk and thrombotic safety. Steroids and certain biologics can impair wound healing, so timing and possible temporary medication adjustments are part of the treatment discussion.
Advanced Considerations for Implant Candidacy
These factors often require additional procedures, lifestyle changes, or long-term commitments. They can affect timing, cost, and the specific surgical approach your dentist recommends.
Previous Dental Treatments
Your past dental work shapes the options your dentist will recommend. Existing crowns, bridges, or root canals near the planned implant site can change implant placement angles or require removal. If you have a failed implant, your dentist will evaluate the cause—infection, overload, or bone loss—and may plan for explantation and site regeneration before placing a new implant.
Prior extractions and the timing since tooth loss matter for bone volume. Long-standing tooth loss often causes ridge resorption; you may need bone grafting or a sinus lift for upper molar sites. If you’ve had periodontal (gum) treatment, share records: a history of treated periodontitis raises the need for strict infection control and closer maintenance after implant placement.
Smoking and Tobacco Use
Smoking directly lowers implant success rates through reduced blood flow and impaired healing. Nicotine constricts blood vessels, slowing bone integration (osseointegration) and increasing risk of infection or implant failure. Many studies show higher marginal bone loss and greater risk of peri-implantitis in smokers versus non-smokers.
Your clinician will likely ask you to quit or reduce tobacco use before surgery and during the healing period—typically at least 2–3 weeks before and several months after placement. Some practices require a longer abstinence or set stricter success expectations. Vaping and smokeless tobacco also affect outcomes and should be disclosed and addressed.
Commitment to Aftercare
Successful implants need ongoing care beyond surgery. You must follow a home hygiene routine: twice-daily brushing, daily interdental cleaning (floss, interdental brushes, or water floss), and possibly adjunctive rinses as directed. Mechanical plaque control around implant restorations prevents mucositis and peri-implantitis.
Regular professional follow-up matters: expect 3- to 6-month recalls initially, with radiographs and probing to monitor bone levels. If you grind your teeth, a night guard can protect implants and reduce biomechanical overload. Be prepared for possible maintenance costs like professional cleanings, prosthetic repairs, or periodic screw retorquing.
Next Steps If You’re Not an Ideal Candidate
You still have practical options to restore function and appearance. Your dentist will outline alternatives and preparatory treatments tailored to your mouth, health, and timeline.
Alternative Tooth Replacement Options
If implants aren’t possible right now, you can choose from several reliable restorations that restore chewing and appearance. Removable partial dentures replace multiple teeth and are relatively quick and inexpensive. They restore basic function and are adjustable if your mouth changes.
A fixed dental bridge spans an area of missing teeth by anchoring to adjacent natural teeth or crowns. Bridges provide a stable bite and a natural look but require altering neighboring teeth. Resin-bonded (Maryland) bridges preserve more tooth structure but suit smaller gaps.
For single-tooth replacement where surgery isn’t an option, a removable flipper offers a temporary aesthetic fix during planning or healing. Ask your dentist about costs, longevity, maintenance needs, and how each option affects future implant placement.
Pre-Implant Procedures and Treatments
You may qualify for implants after targeted treatments that address the issues preventing surgery now. Common preparatory procedures include bone grafting to rebuild jaw volume and sinus lifts to increase bone height in the upper back jaw. Both procedures increase implant success by providing a solid foundation.
If periodontal disease or infected teeth block implant placement, your dentist will treat infection with deep cleanings, root planing, or extractions. Smoking cessation, improved diabetes control, and nutritional optimization often form part of the plan because they improve healing and reduce complications.
Discuss timelines and staged approaches. Some grafts heal in 3–6 months before implant placement; others allow simultaneous graft-and-implant surgery. Your dentist will give specific estimates, expected outcomes, and costs so you can make an informed choice.