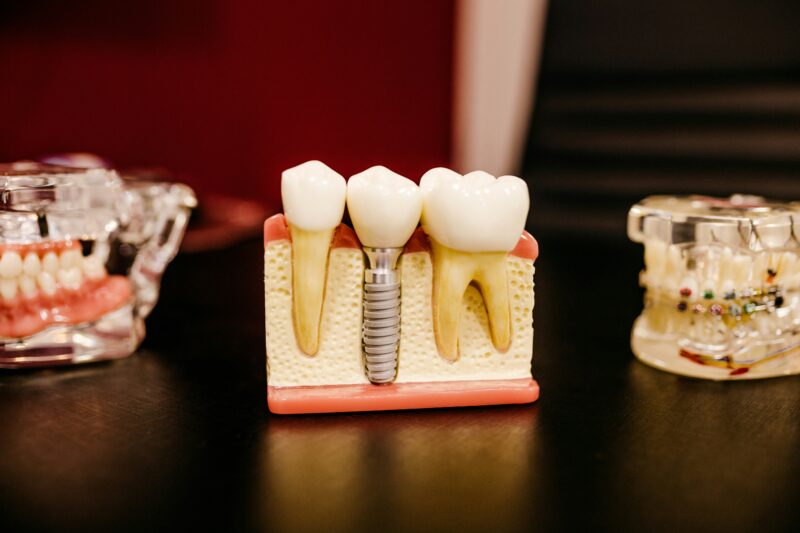
Considering dental implants after 60 can feel like a big decision, but you can often get stable, long-lasting tooth replacement that restores chewing, speech, and confidence. Many older adults exploring dental implants in High Point, NC qualify for the procedure, and age alone usually isn’t a disqualifier — what matters more are your overall health, bone condition, and medical history.
This article walks through the benefits you can expect, how candidacy gets assessed, what the procedure and recovery involve, and the risks and aftercare that affect long-term success. You’ll get clear, practical information to help you decide whether implants fit your goals and health situation.
Benefits of Dental Implants for Older Adults
Dental implants restore chewing, speech, and facial support while reducing the need for frequent adjustments and denture-related adhesives. They directly address bone loss, loose prostheses, and the day-to-day limits that missing teeth create.
Improved Quality of Life
You regain the ability to chew a wider variety of foods, including firmer proteins and raw fruits and vegetables, which helps maintain nutrition and energy. Implants feel and function more like natural teeth, reducing the slipping, clicking, and sore spots that often come with removable dentures.
Speaking and social confidence often improve because implants don’t shift during conversation or laughter. You also avoid daily removal and messy adhesives, so your routine becomes simpler and more comfortable.
Enhanced Oral Health
Implants replace tooth roots with a titanium post that integrates with bone, preserving jaw structure and preventing the accelerated bone loss that follows tooth extraction. Unlike bridges, implants don’t require cutting adjacent healthy teeth for support, so you protect remaining natural teeth.
You can clean around an implant-supported crown similarly to a natural tooth—brushing and flossing—so oral hygiene is straightforward. Your dentist may recommend periodic professional cleanings and checks to monitor tissue health and implant integration.
Long-Term Stability
Dental implants offer durable support: many modern implants last decades with proper care, reducing the need for frequent remakes or relines common with dentures. The fixed nature of implants maintains consistent bite force and chewing efficiency over time.
Risk factors—poor bone volume, uncontrolled diabetes, or heavy smoking—can affect success rates, so your clinician will evaluate and manage these before treatment. With appropriate planning (bone grafting if needed) and maintenance, implants provide a predictable, long-term tooth replacement option.
Candidacy and Assessment After Age 60
You will be evaluated on bone quantity and quality, overall medical status, and your dental history. These three areas determine whether implants are feasible, whether preparatory procedures are needed, and what risks to expect.
Evaluating Bone Health
Your jawbone must provide enough height and width to hold an implant and integrate with it. Dentists use CBCT scans or panoramic X-rays to measure bone volume and density at the implant site.
If bone is insufficient, your options include bone grafting, sinus lift (upper back jaw), or using narrower or angled implants; each option changes healing time and cost.
Look for signs of bone loss from long-term tooth absence or periodontal disease. Smoking and osteoporosis medications (bisphosphonates) can affect bone healing; your clinician will factor those into risk calculations.
Your dentist will also check adjacent teeth and bite forces to choose implant size and location that minimize overload and support long-term success.
Medical Considerations for Seniors
Your general health and medications influence healing and infection risk. Conditions such as uncontrolled diabetes, bleeding disorders, or immune suppression require stabilization before implant surgery.
Bring a current list of prescriptions and supplements; anticoagulants, corticosteroids, and some osteoporosis drugs may need coordination with your physician.
Age itself is not a contraindication, but frailty and mobility issues can affect post-op care and follow-up visits. Expect preoperative clearance if you have significant cardiac, pulmonary, or neurologic disease.
Your care team will balance the benefits of implants against anesthesia risks, ability to maintain oral hygiene, and the practicality of multiple appointments.
Dental History and Oral Conditions
Your history of periodontal disease, number and pattern of missing teeth, and prior extractions guide treatment planning. Active gum disease must be controlled before implant placement to reduce failure risk.
Evaluate existing restorations, occlusion (how your teeth meet), and bruxism (tooth grinding); these factors determine implant design, the need for protective night guards, and whether multiple implants or fixed/detachable prostheses suit you.
Previous radiation to the head/neck or recurrent infections require specialized protocols. Your dentist will document saliva flow, mucosal health, and prosthesis fit to ensure long-term maintenance is realistic for your lifestyle and manual dexterity.
What to Expect from the Dental Implant Process
You will go through a structured path: an evaluation to confirm candidacy, a staged surgical plan tailored to your bone and health status, and a predictable recovery with follow-up visits for monitoring and restoration. Costs, timelines, and any additional procedures will be clarified early so you can plan.
Consultation and Planning
Your first visit includes a medical and dental history review, focusing on conditions like diabetes, osteoporosis, and blood-thinning medications that affect healing. Expect a clinical exam plus imaging—typically a panoramic X-ray and a CBCT scan—to measure jawbone thickness and map nerve and sinus locations.
The dentist or oral surgeon will discuss implant types (single, multiple, or implant-supported dentures), whether bone grafting or sinus lifts are needed, and a proposed timeline. They will review anesthesia options, estimated costs, and insurance or financing. You should receive a written treatment plan with step-by-step stages, appointment estimates, and any pre-operative instructions such as stopping specific medications.
Surgical Procedure Steps
On surgery day, you will receive local anesthesia and, if chosen, sedation or general anesthesia for comfort. The surgeon makes a small incision in the gum, drills a pilot hole in the jawbone, and places the titanium implant body flush with the bone. A healing cap or temporary crown may be placed, depending on stability and immediate load decisions.
If bone grafting or sinus augmentation is required, the graft may be performed at the same visit or as a separate procedure weeks to months earlier. Typical single-implant placement takes 45–90 minutes; multiple implants or grafts take longer. You will get clear post-op instructions, prescriptions for pain control and sometimes antibiotics, and a schedule for suture removal if non‑resorbable stitches were used.
Recovery Timeline
Initial recovery usually lasts 7–14 days: swelling and mild pain peak in the first 48–72 hours and improve with cold packs, rest, and prescribed or over‑the‑counter pain relievers. You should stick to a soft-food diet for the first week and avoid strenuous activity that raises blood pressure.
Osseointegration—the implant fusing to bone—takes 3–6 months depending on bone quality and any grafts. During this period, you will return for periodic checks and X-rays to verify stability. After successful integration, your dentist will place an abutment and final crown or attach the prosthesis; that restorative appointment usually requires one or two visits spaced a few weeks apart. Maintain good oral hygiene and follow maintenance visits every 3–6 months to protect long‑term success.
Risks, Aftercare, and Longevity
You’ll face specific risks tied to health and bone quality, require clear post‑procedure care steps, and can take concrete actions to extend how long implants last.
Potential Risks for Older Adults
Age alone doesn’t bar you from implants, but medical conditions increase complication risk. Diabetes with poor blood sugar control raises infection and healing problems. If you take bisphosphonates or certain anticoagulants, discuss timing and management with both your dentist and prescribing physician.
Reduced jawbone density can lead to implant failure or require bone grafting before placement. Smoking and heavy alcohol use also impair healing and raise the chance of implant loosening. Surgical risks include infection, nerve injury (numbness/tingling), and sinus perforation for upper jaw implants. Ask your clinician for an individualized risk assessment, including imaging (CBCT) and medical clearance when needed.
Post-Procedure Care
Follow prescribed antibiotics and pain control exactly as directed to reduce infection and discomfort. Maintain gentle oral hygiene: use a soft-bristled brush, chlorhexidine rinse if recommended, and avoid aggressive flossing directly at the surgical site until your clinician clears it.
Limit hard, chewy foods for the first 6–8 weeks or until your clinician confirms osseointegration. Avoid smoking and vaping during healing; even short relapses raise failure risk. Attend all follow-up visits at 1 week, 6–8 weeks, and 3–6 months (or as scheduled) so your provider can check soft tissue health, stability, and bite alignment.
Ensuring Implant Longevity
You can improve implant survival by controlling modifiable health factors. Keep HbA1c within your provider’s target if you have diabetes and maintain good nutrition to support bone healing. Stop smoking and minimize alcohol to improve long-term outcomes.
Adopt a maintenance routine: professional cleanings every 3–6 months if you’ve had periodontal disease, otherwise every 6–12 months. Use interdental brushes sized for the implant area to remove plaque around the abutment. Report any loosening, persistent pain, swelling, or new sensitivity promptly—early intervention often prevents implant loss.