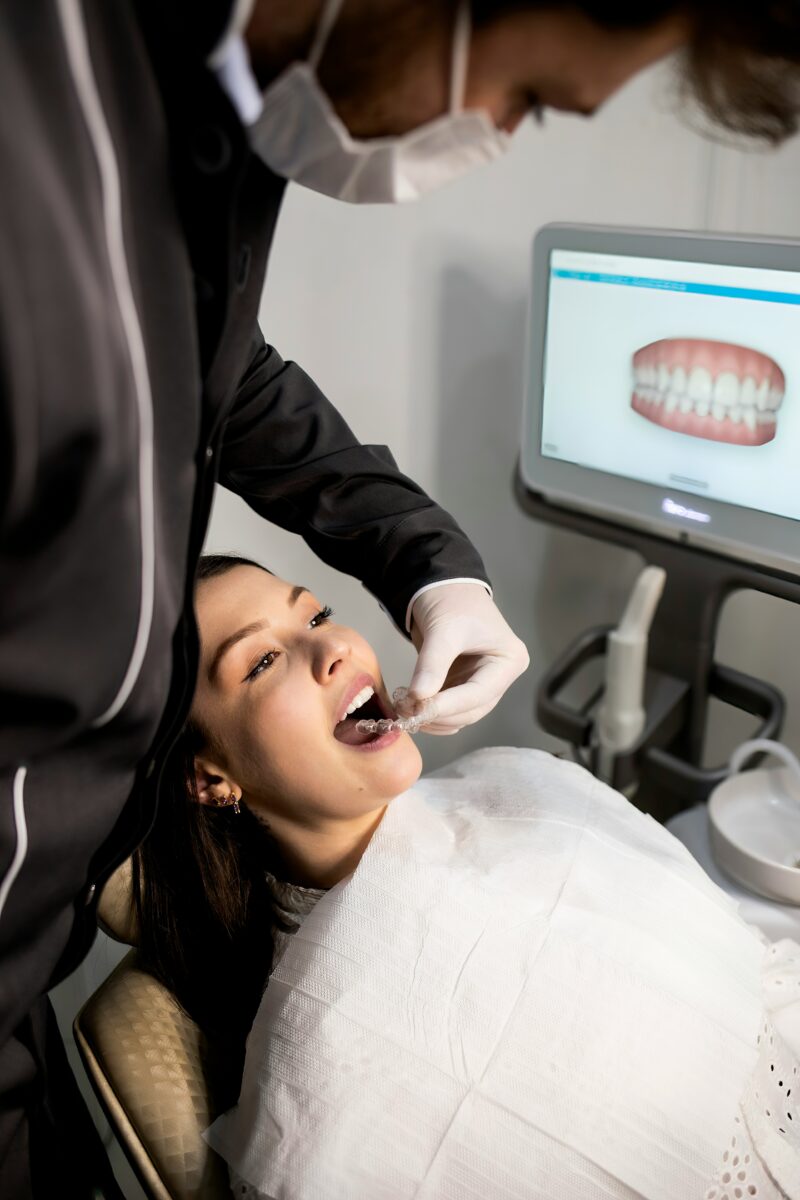
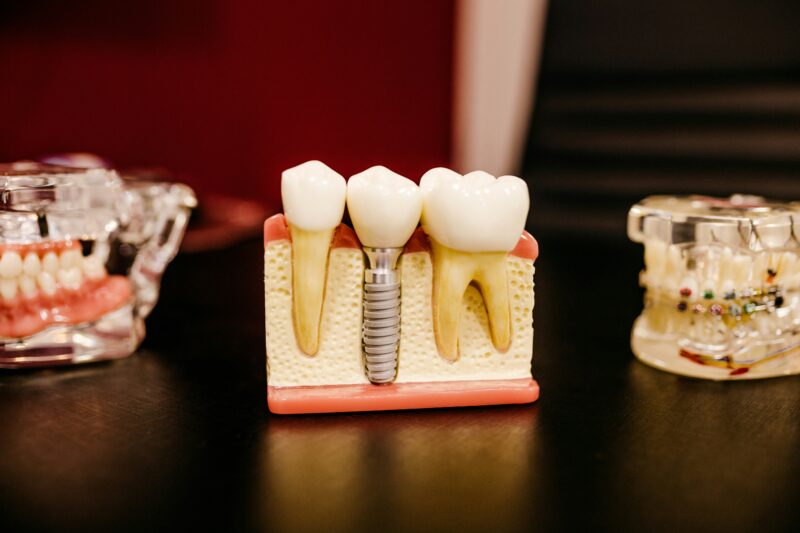
Dental implants give you a stable, natural-feeling tooth replacement, but they need the same consistent care as natural teeth to last. For anyone considering dental implants in Ocala, FL, following a simple daily routine — effective brushing, flossing around the implant, and using recommended interdental tools — will greatly reduce the risk of complications and extend the life of your implant.
You’ll also learn when to see your dentist for professional maintenance, which lifestyle habits to adjust, and how to spot early signs of trouble so you can act quickly. This guide breaks those steps into practical actions you can start using today to protect your smile and your investment.
Daily Care Essentials for Dental Implants
Keep plaque off implant crowns and protect the gum tissue and bone around the implant with consistent brushing, the right products, and daily interdental cleaning. Small, deliberate habits—done every day—prevent most implant-related problems.
Brushing Techniques for Implants
Use a soft-bristled toothbrush or an electric brush with a soft head to clean implant crowns and surrounding gum tissue twice daily. Hold the brush at a 45° angle to the gum line and use gentle circular motions; avoid heavy scrubbing that can irritate the tissue around the implant.
If you use an electric brush, move it slowly along each tooth and the implant restoration for 2 minutes total. Pay extra attention to the area where the crown meets the gum—biofilm collects there. Rinse with water after brushing and inspect the crown for food debris or discoloration.
For multi-unit restorations (bridges or All-on-X), brush around and under the prosthesis carefully. Use a single-tuft or end-tuft brush to reach tight spots and the abutment connection.
Selecting Implant-Safe Oral Care Products
Choose non-abrasive toothpaste to avoid scratching titanium or ceramic crowns; look for products labeled “low-abrasivity” or with a Relative Dentin Abrasivity (RDA) under 70. Avoid whitening pastes with strong abrasives or peroxide concentrations that can affect crown finish.
Pick an antimicrobial mouthwash containing chlorhexidine only if your dentist recommends short-term use; long-term chlorhexidine can stain and alter oral flora. Alcohol-free antiseptic rinses (cetylpyridinium chloride or essential-oil formulations) work for daily use without drying tissues.
Use a soft-bristled manual or soft-headed electric toothbrush. For interdental spaces, choose between waxed floss, floss threaders, interdental brushes with nylon bristles, or water flossers based on the implant type and your dexterity.
Flossing and Interdental Cleaning
Floss around implants once daily to remove biofilm from the implant–gum interface. If you have a single implant crown, use implant-safe floss (waxed or PTFE) and slide gently up and down along the side of the crown and under the contact point. Avoid sawing motions that can fray the floss and lodge fibers.
For fixed bridges, implant-supported prostheses, or tight contacts, use a floss threader or superfloss to pass floss beneath the restoration. Interdental brushes sized to the papillary space work well for wider embrasures; choose nylon filaments and avoid metal cores that can scratch.
Consider a water flosser set to a gentle pressure setting for daily use if you struggle with conventional floss. Use steady, directed pulses along the gumline and under prostheses to dislodge debris and reduce bleeding.
Professional Maintenance and Regular Check-Ups
Regular professional care preserves implant function and detects problems early. Expect scheduled cleanings, soft-tissue checks, and occasional X-rays to monitor bone and prosthetic stability.
Importance of Professional Cleanings
Professional cleanings remove hard-to-reach plaque and calculus around implant abutments and beneath prosthetic margins. Hygienists use implant-safe instruments—typically plastic, titanium, or specially coated scalers—and ultrasonic tips designed for implants to avoid scratching the implant surface.
During a cleaning, the clinician also evaluates your home-care technique and may recommend changes, such as switching to a particular interdental brush size or using a water flosser for difficult areas. Cleanings usually occur every 3–6 months depending on your inflammation levels, history of peri-implant disease, and the type of restoration you have.
Monitoring Implant Health with Dental Visits
Dental visits track soft tissue health, pocket depth, and bone level around implants. Clinicians measure peri-implant probing depths carefully and compare them to baseline values established after prosthesis delivery. They also inspect for bleeding on probing, suppuration, and mobility—each sign warrants closer follow-up.
Periodic radiographs (periapical or bitewing) help detect early bone loss that you won’t feel. Your provider may increase visit frequency if they see progressive bone loss, persistent inflammation, or mechanical wear on the restoration.
Role of Your Dentist in Implant Longevity
Your dentist coordinates long-term care, balancing surgical, restorative, and periodontal perspectives. They evaluate occlusion and adjust bite forces that could overload the implant, which helps prevent screw loosening and prosthetic fracture.
They also set the maintenance interval and refer you to a periodontist or oral surgeon when persistent infection, crestal bone loss, or complex complications arise. If prosthetic parts wear or break, your dentist will repair or replace components and document changes to maintain an accurate clinical baseline.
Lifestyle Considerations for Implant Longevity
Small daily choices around what you eat and whether you use tobacco have measurable effects on gum health, bone stability, and the lifespan of your implants. Focus on foods that support healing and avoid substances that impair blood flow or increase infection risk.
Dietary Choices and Their Impact on Implants
Choose nutrient-dense foods that promote bone and gum health. Prioritize calcium-rich dairy or fortified alternatives, lean proteins for tissue repair, and vitamin C–rich fruits and vegetables to support collagen and immune function. If you take supplements (calcium, vitamin D), follow your dentist’s guidance to avoid interactions with medications.
Limit hard, sticky, or very chewy foods—ice, hard candy, and tough jerky can stress crowns or abutments and increase the chance of restoration damage. Cut tough items into small pieces and chew on the opposite side when possible. Minimize frequent snacking on sugary or acidic foods and drinks to reduce plaque build-up around implant margins.
Hydrate well; dry mouth heightens the risk of plaque and peri-implant disease. If you use acidic beverages like soda, rinse with water afterward and avoid swishing liquids around the implant site. Discuss any special diet (e.g., bariatric, vegan) with your dental team to ensure adequate nutrient intake for implant support.
Tobacco Use and Dental Implant Health
Tobacco use—cigarettes, cigars, vaping, and smokeless tobacco—directly increases the risk of implant failure. Nicotine constricts blood vessels, reducing blood flow to the gums and bone and impairing healing after implant placement. This effect raises the chance of infection and bone loss around the implant.
If you smoke or use nicotine products, the best step is to stop before surgery and remain smoke-free afterward. Even cutting back lowers but does not eliminate risk. Tell your clinician about your tobacco use so they can plan additional monitoring, possible prophylactic measures, and tailored hygiene instructions.
Consider counseling, nicotine-replacement therapy, or prescription medications to quit. Your dental team can coordinate with your primary care provider for cessation support, which improves implant success rates and overall oral health.
Recognizing and Preventing Potential Complications
You should watch for specific symptoms and adopt proven habits that reduce the chance of infection, mechanical failure, and bone loss. Prompt action and routine maintenance are the two most effective defenses.
Identifying Early Signs of Implant Issues
Look for redness, swelling, or bleeding around the implant site during brushing or flossing. These are common early signs of peri-implant mucositis and should prompt a hygiene check with your dental team.
Note any persistent pain, pressure, or discomfort that does not improve after a few days. Acute or worsening pain can signal infection, implant instability, or problems with the restoration fit.
Pay attention to changes in bite or mobility of the crown, bridge, or abutment. Even slight loosening or a feeling that your teeth don’t meet properly can indicate mechanical failure or bone loss beneath the implant.
Monitor chronic bad taste or persistent bad breath despite good oral hygiene. These symptoms often point to infection or trapped debris around the implant that needs professional cleaning.
Preventive Measures to Reduce Risks
Clean around implants at least twice daily using a low-abrasive toothpaste and a soft-bristled brush. Use an interdental brush (nylon, size matched to the space) or floss specifically designed for implants to remove plaque from between the implant and adjacent teeth.
Schedule professional implant maintenance every 3–6 months, or as your dentist recommends. Hygienists use non-metallic instruments and ultrasonics designed for implants to remove hardened deposits without damaging the implant surface.
Avoid smoking and limit excessive alcohol; both increase the risk of impaired healing and peri-implant disease. If you grind your teeth, ask about a night guard to prevent overload and mechanical failure.
Report any early warning signs immediately and keep all follow-up and radiographic appointments. Timely intervention—professional cleaning, adjustment of the restoration, or targeted antibiotics—can stop progression and preserve the implant.