Lipids are important in the production of vitamin D. They serve as the building blocks for the molecules that help make up the hormone and its active form, calcitriol. This article will provide an overview of the different lipids involved in vitamin D production, the roles they play in the body, and their sources in the diet.
Which lipid is part of vitamin d
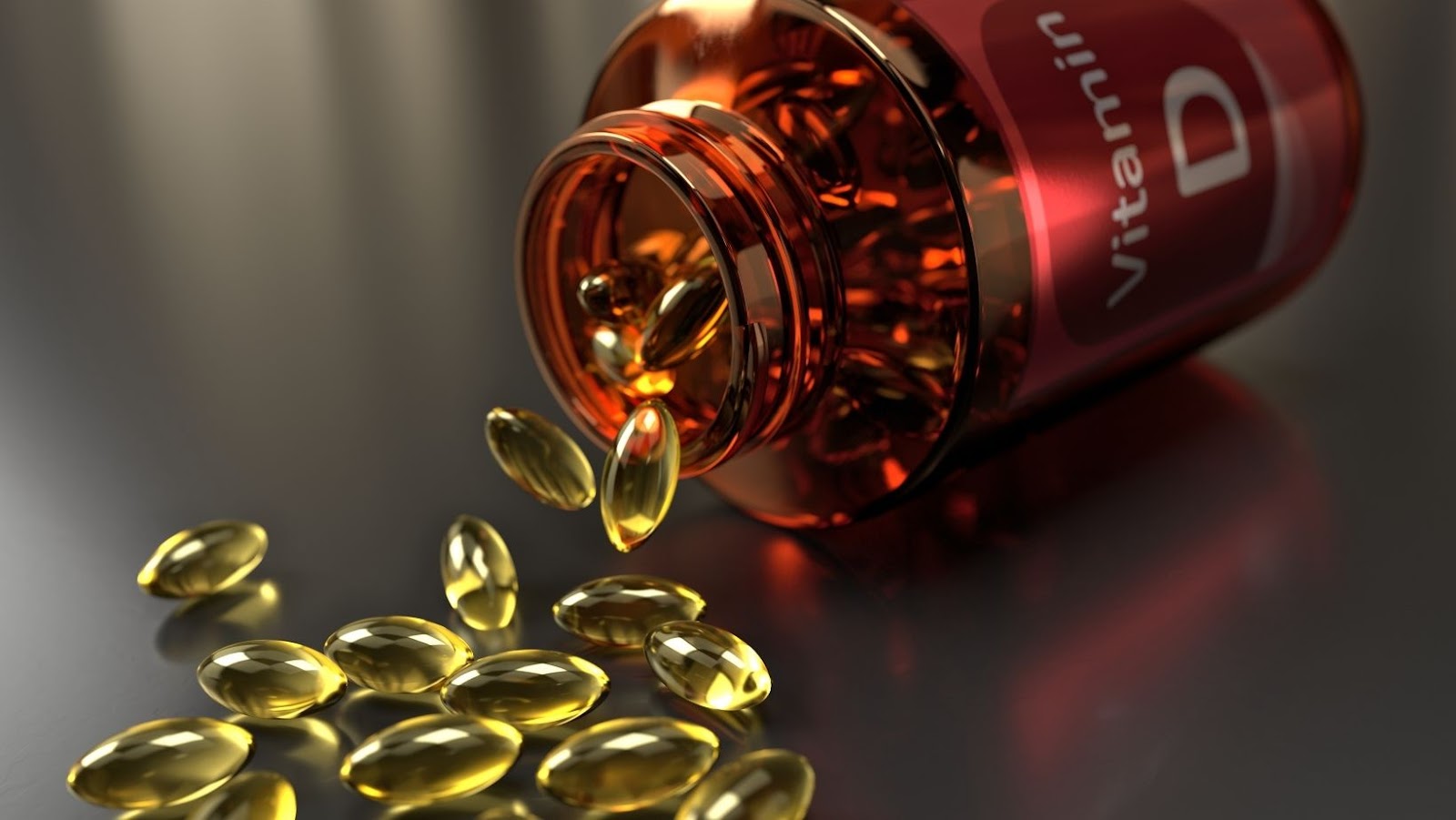
Vitamin D, a fat-soluble vitamin typically found in food, aids the absorption of calcium in the gut and supports bone health. It is also used to promote healthy metabolic function, immune systems and cardiovascular health. In the body, Vitamin D is created when ultraviolet rays from the sun trigger reactions in various lipids found naturally in the skin.
There are two active forms of Vitamin D – Vitamin D2 (also called ergocalciferol) and Vitamin D3 (also called cholecalciferol). These two forms are essential for a number of bodily functions as they help with calcium absorption, healthy bones and muscle growth.
Vitamin D3 is formed from a compound called 7-dehydrocholesterol found in our skin that reacts with ultraviolet light to produce an activated form cholecalciferol or Vitamin D3; this reaction occurs mainly when we are exposed to sunlight. The production process of Vitamin D2 follows a similar pathway but involves ergosterol as its source which is mostly found from plants or fungal sources (including mushrooms) rather than sunlight like vitamin D3 does.
Most multivitamins available on the market contain one or both types of dietary supplements as well as vitamins A, C and E. In addition to these essential vitamins, Vitamin E has been shown to be important for cell division too, so many products will include additional amounts of it where possible. Eating foods rich in these vitamins such as dairy products and eggs can increase our daily intake significantly if taken in moderation – eating fish such as salmon also helps our body absorb more efficiently due to its high content of omega 3 fatty acids .
Role of Lipids in Vitamin D Production
Lipids play a critical role in the production of Vitamin D, an essential vitamin that aids in bone health, cell growth and immune system function. Vitamin D production is complex and requires the involvement of several key lipids.
Cholesterol, one of the most important lipids for producing vitamin D, is found in skin cells and liver cells, and it helps maintain healthy levels of calcium in the body. When cholesterol from dietary sources or from the body is exposed to sunlight, it reacts with ultraviolet light to form pre-vitamin D3. Pre-vitamin D3 then moves to the liver where it is transformed into a form called 25-hydroxyvitamin D3 or calcidiol. Finally, this compound is converted into its active form 1α-25 dihydroxyvitamin D3 or calcitriol within renal tubules of the kidney.
It is also worthy to note that there are two other types of lipid molecules which play an important role in vitamin absorption – Calcium Phosphate Liposomes and Sterols. The former are composed of lipids known as phospholipids which bind with calcium and phosphorus inside intestinal cells helping facilitate their absorption into bloodstreams while sterols are used by enterocytes as carriers that possess a hydrophilic head structure surrounding a hydrophobic tail structure to facilitate transfer across cell membranes – both play a similar role in aiding transcellular transportation for vitamins like Vitamin A & E limiting their degradation before getting absorbed by epithelial cells present in duodenum’s mucosa walls..
Lipids and Vitamin D
Vitamin D is an essential nutrient that is required for healthy bone growth and muscle function, and it is largely produced in response to exposure to sunlight. One important lipid that plays a role in the production of Vitamin D is 7-dehydrocholesterol. This lipid is even referred to as “pro-vitamin D3” due to its role in the production of Vitamin D3. Let’s take a closer look at the role of lipids in the production of Vitamin D.
Types of Lipids Involved in Vitamin D Production
Vitamin D is created from cellular complexes known as lipids – which are a group of fats, waxes, sterols, and fat-soluble vitamins. Vitamin D is created in two pathways: one in the skin with exposure to sunlight and the other by ingestion of food or supplements.
The two main types of lipids involved in vitamin D production are cholesterol and fatty acids. Cholesterol is the most important lipid for vitamin D production due to its role in facilitating metabolic activities. Cholesterol helps create previtamin D3 from ultraviolet light and serves as a substrate for pre-vitamin D3 to transform into an active form of vitamin D3 (dihydroxyvitaminD3).
A variety of fatty acids have been found to be important in vitamin D production such as palmitic acid, oleic acid, linoleic acid, lauric acid, myristic acid, stearic acid and arachidonic acid. These essential fatty acids are needed for the creation of hormone-like compounds called eicosanoids that help control reactions within cells when they come into contact with UV rays. These eicosanoids then facilitate the transformation from provitamin D3 to active forms of vitamin D3. In addition to allowing for metabolic transformations within cells, these fatty acids serve as a blood reservoir for storing active forms of vitamin D3 or dihydroxyvitaminD3 for use at later stages.
When combined with adequate exposure to sunlight (which contains ultra violet radiation composed mostly of UVA/UVB) both cholesterol and fatty acids facilitate the conversion from an inactive form (cholecalciferol or pre-vitaminD) into its active form known as dihydroxyvitaMinD or calcitriol. This physiological conversion represents an important aspect of human health and is essential for proper absorption processes related to calcium absorption leading to potential increases in bone density integrity, improved neurological processes such as cognitive development in infants/children; it also has been linked with some cancer prevention mechanisms.
Function of Lipids in Vitamin D Production
Vitamin D exists as a family of fat soluble vitamins and is responsible for several physiological activities. This includes aiding in the absorption of calcium, helping to maintain bone health, improving immunity and regulating cell growth. Some of these functions are mediated by lipids – molecules consisting of glycerol and fatty acid chains that have a variety of biological roles.
To understand the role of lipids in vitamin D production, it is necessary to look at two types – cholesterol and triglycerides. Cholesterol plays a key role in the synthesis and absorption of vitamin D. It helps to carry vitamin D throughout the body, as well as forming part of its structure. Triglycerides are molecules made up of fat molecules linked to glycerol — they are derived from dietary sources such as meat, fish, dairy products, avocado and nuts.
The triglycerides act as carriers for vitamins A and D; they form part of the chemical structures which aid in the transport of these fat-soluble vitamins through the body. In addition to this, cholesterol-rich lipoproteins have specific receptors which help to absorb dietary vitamin D into the circulation so that it can be used for metabolic purposes. Without lipids being involved in this process, vitamin D would not be able to be effectively absorbed into our bodies or utilised properly. Therefore lipids play an essential role in maintaining normal levels of Vitamin D in our body’s system.
Vitamin D Metabolism
Vitamin D is an essential nutrient for human health. It is involved in calcium metabolism, bone growth, immune system regulation, and many other important functions. It is essential for the proper absorption of dietary calcium and phosphorus. Vitamin D is produced when ultraviolet rays from the sun interact with cholesterol-containing molecules in the skin. This interaction is necessary for the conversion of cholesterol to the active form of vitamin D, which is known as cholecalciferol.
Vitamin D Synthesis
Vitamin D is produced endogenously (by the body) when ultraviolet B (UVB) wavelengths of sunlight penetrate the skin and interact with a lipid called 7-dehydrocholesterol. The UVB radiation causes this lipid to form vitamin D3, which then undergoes several transformations in the liver and kidneys in order to become active vitamin D, also known as calcitriol. Biologically active vitamin D helps regulate calcium levels in the body by controlling movement of calcium from bones into blood and intestine; it may also contribute to increased cell differentiation.
The process begins when UVB radiation penetrates skin cells and is absorbed by the 7-dehydrocholesterol molecule, a member of the sterol family of lipids that exist on the cellular membranes. When UVB radiation interacts with this molecule, it provokes a reaction resulting in formation of previtamin D3 (proVD3). Due to its high stability, proVD3 can be found in skin or circulate in the bloodstream. Eventually it undergoes transformation into vitamin D3 via two different UVR-dependent mechanisms: isomerization within cells or direct photolysis outside cells. Vitamin D3 then travels through the bloodstream unprotected until being taken up for further metabolism by liver or kidneys via specific transporters called megalin and cubilin colin receptors.
In both organs, vitamin D3 undergoes enzymatic hydroxylation catalysed by cytochrome P450 enzymes – 25-hydroxyvitaminD 3 starts forming by addition three hydroxyl groups (-OH) at positions C25 position (forming 25(OH)D 3); 1α-hydroxylase adds an additional -OH at C1 position forming 1α ,25-dihydroxyvitamin D3 – calcitriol– which represents an active form of vitamin d that mediates maximum biological activity. All these biochemical processes are modulated metabolic pathways involving intervening factors such as epidermal growth factor or low dietary phosphate intake all have an important role determining final concentrations of calcium and ions entering homeostasis regulation systems within organisms..
Vitamin D Transport
Vitamin D is an essential nutrient found in both dietary sources and produced as a result of UVB exposure on the skin. Vitamin D plays a vital role in absorbing calcium, regulating the immune system and contributing to optimal health.
To be utilised by the body, vitamin D first needs to be activated through hydroxylation. This process occurs in the liver and kidney involving several enzymes that act as catalysts. In order to reach these enzymes, vitamin D must be transported within cells using lipids such as cholesterol. Cholesterol is not only necessary for synthesising Vitamin D, but also acts as an intracellular carrier molecule sending it where it’s needed.
The lipid which helps transport vitamin-D is low-density lipoprotein (LDL). LDL binds to Vitamin-D leading it on its journey through the bloodstream towards its target locations including the liver, where Vitamin D is hydroxylated, and other tissue sites such as skeletal muscle that require Vitamin-D for maintenance or growth. Without adequate levels of cholesterol or LDL molecules present in circulation, our bodies would not be able to utilise this critical nutrient leading to long term deficiencies with accompanying health risks.
Vitamin D Activation
Vitamin D is a fat-soluble vitamin obtained from diet or generated in the skin by the action of ultraviolet rays of sunlight. It plays an important role in calcium homeostasis and bone metabolism, functioning as an important regulator of deposition of calcium and phosphorus in bones.
Vitamin D is mainly metabolised by two hydroxylations catalysed by specific enzymes occurring at successive steps: first, within the liver (hydroxylation step), where 25-hydroxyvitamin D (25OHD) is formed; secondly, within the kidney (activation step), where 1,25 dihydroxyvitamin D (1,25-(OH)2D3) is formed. This active form binds to its receptor (VDR), which regulates gene transcription that involve calcium homeostasis and bone metabolism.
Conclusion
After examining the role of lipids in vitamin D production, it’s clear that certain lipids are essential for the functioning of vitamin D. Cholesterol is the key lipid which is part of vitamin D, and its ability to bind with other compounds to form the necessary precursor molecules is essential for the production of vitamin D. Additionally, cholesterol is also required for the binding of vitamin D to various proteins for transport and storage in the body.
Summary of Findings
The research into the role of lipids in vitamin D production has shown that lipids, such as fatty acids and sterols, play an important part in the synthesis of active vitamin D. The two main types of fat-soluble vitamins, retinol (vitamin A) and D3, both depend on certain lipids for their absorption. Specifically, long-chain fatty acids from both dietary fats and cholesterol must be present for adequate absorption and transport of vitamin D in humans. Further research should be conducted to determine which lipid is most important for optimal levels of vitamin D production in the human body. Additionally, further studies are needed to determine how various lipids interact with each other and with vitamin D during the absorption process.
Implications for Future Research
It is clear that additional research is needed to more fully understand the role of lipids in vitamin D production. While the role of cholesterol in vitamin D synthesis has been established, other potential players remain underexplored. Further study may be necessary to determine the exact role that non-cholesterol lipids may play in vitamin D synthesis and how they interact with existing cholesterol pathways.
Additionally, it would be beneficial to explore variations between different age groups and dietary habits, as this can influence overall vitamin D status. To this end, population-based studies should be conducted to further appreciate how lipid composition relates to different health states as well as response to supplementation strategies.
Ultimately, a better understanding of the role of lipids in vitamin D production could provide novel insights into how varying lipid concentrations might contribute to or protect against different disease states. This information could then be used for targeted supplementation strategies or dietary changes better suited for specific needs.